Saturated Fat
Dean Ornish, in an opinion article in The New York Times wrote that “…low-carb, high-animal-protein diets promote heart disease,” and he praises the virtues of plant-based diets free of “harmful fats” which he defines as trans-, saturated, and hydrogenated fats (Ornish, 2015). He goes on to demonize egg yolks with the unsubstantiated claim that choline increases the risk of heart disease! Articles like this make people afraid of nutrient-dense foods that have nourished humans for centuries. Perhaps the anti-meat campaign emerges from a misguided concern for the environment; a pushback against the environmentally destructive agricultural practices integral to the CAFO production model. Instead of encouraging readers to seek sustainably raised meats, Ornish condemns all animal production models, saying: “Livestock production causes more disruption of the climate than all forms of transportation combined,” a myth that has been thoroughly debunked by Allan Savory (Savory, 2013), Joel Salatin (Salatin, 1995, p. 193), and others who advocate and demonstrate a sustainable model for agriculture. Ornish is one of many cacophonous voices in a choir of anti-traditional food rhetoric. The American Heart Association and the US Government’s dietary recommendations have similarly been critical of saturated fat, while more lenient to the liquid oils (USDA, HHS, 2010), and as a result, seed oil use has soared in recent decades, to the detriment of our collective health.
How did saturated fats get their scandalous reputation? The lipid hypothesis was postulated in the 1950s by Ancel Keys. He proposed that fat and cholesterol in the diet is a causal factor in coronary artery disease. A few other studies around this time showed that the increased consumption of plant products and avoidance of animal fats reduced serum cholesterol. Some early researchers discovered that plaque in the arteries contains cholesterol, so it seemed logical to conclude that cholesterol clogs arteries in the way that grease clogs a pipe. Unfortunately, this is a hopelessly simplistic and erroneous explanation of a very complex disease process. But its simplicity makes it hard to refute in public opinion. A couple decades earlier in the early 1900s, Nikolaj Anitschkov conducted an experiment in which he fed massive amounts of cholesterol to rabbits, which afterwards developed a condition similar to CVD (cardiovascular disease) in humans (Konstantinof, Mejivoi, & Anichkov, 2006). This study seemed to point to dietary cholesterol in causing the artery disease. A later variation of this study found that injecting cholesterol directly into the veins of rabbits did not cause disease. The lipoprotein molecule had not been discovered at this time, and the contribution of oxidative stress on CVD was not understood. The lipid-heart hypothesis was not well-received at the time, but began to be accepted when drug manufacturers developed drugs to lower blood cholesterol, the United States has become a major producer of the yellow vegetable seed oils, and the food industry found a niche in low-fat products that are reported to be healthy.
The consumption of saturated fats and cholesterol does increase serum cholesterol, at least in the short term. It also has been long known that certain polyunsaturated fats (the essential fatty acids) are able to lower cholesterol. And because elevated cholesterol is associated with cardiovascular disease, it’s easy to make the short intellectual jump to conclude that polyunsaturated fats are heart-healthy, and saturated fats are detrimental. One early study was performed to prove the efficacy of treating heart disease with unsaturated fats. Volunteers were given 80g/day of either corn oil, olive oil, or no oil. Instead of preventing heart disease, the study group had significantly more incidence of heart disease, with the corn oil group having the highest risk of all (Rose, Thomson, & Williams, 1965). The study concludes with:
It is concluded that under the circumstances of this trial corn oil cannot be recommended in the treatment of ischaemic heart disease. It is most unlikely to be beneficial, and it is possibly harmful.
It is an understatement to say that corn oil isn’t beneficial for treating heart disease, it actually contributes to it! Other studies have shown similar results, including the Sidney Diet Heart Study: an intervention study which found that replacing dietary saturated fat with linoleic acid increased death rates from all causes, including CVD and CHD (Ramsden, et al., 2013). Although certain polyunsaturated fats (PUFAs) are essential in the diet, only very small amounts are necessary. The more unsaturated the fat, the greater the chance that it will become oxidized, generating free radicals and advanced glycation end products, which damage tissues. The membranes of lipoproteins are made from fats, and if these fats oxidize, they are less able to activate the LDL receptor, and ultimately damage the delicate lining of blood vessels and arteries, leading to disease. A high PUFA diet promotes oxidative stress, while fully saturated fats are resistant to oxidation.
There continues to be a debate about the health benefits of fats, and conflicting studies are trumpeted by both sides that muddy the waters of public opinion, but people are more likely to believe a study that reinforces a previously held belief. The American Journal of Clinical Nutrition published an analysis of 11 studies that concludes “…replacing SFA intake with PUFA….prevents CHD over a wide range of intakes and among all middle-aged and older women and men” (Jakobsen et.al., 2009). They explain in a later article that “Most polyunsaturated fatty acids in the diet are of the omega-6 (n–6) type. These lower serum LDL cholesterol and, in clinical trials, the risk of heart disease” (Katan, 2009). The conclusion of this study is dubious, if not outright deceptive. I wasn’t able to get full access to the eleven studies that were cited by Jakobsen et.al., so my ability to scrutinize is limited, but “clinical trials” in many cases are observational trials based on questionnaires, which depends on self-reported information. To question people about their saturated fat and cholesterol intake might simply segregate health-conscious people from those eating the standard American diet, full of cheeseburgers and donuts. One of the studies cited by the review is the Adventist Health Study which concludes that “the frequent consumption of nuts may protect against risk of CHD events” (Fraser, Sabate, Beeson, & Strahan, 1992). So people who report consuming a lot of nuts have lower CHD risk, which seems reasonable, but the findings are extrapolated to suggest that the PUFA oils in those nuts protect from heart disease. Might other factors be involved? Nuts are a good source of many types of fats as well as essential minerals and antioxidants, and the PUFAs in a whole-food form are much more protected from oxidation than that of the yellow cooking oils. Or might those people eat nuts instead of snacking on pizza and Twinkies? Fast food is a big player here. For many Americans, saturated fat in the diet comes from hamburger, a processed meat which is typically consumed with a serving of white flour, potatoes fried in rancid yellow oil, and maybe a sugary beverage or two. A study here shows that Adventists who are vegetarians are less likely to smoke, drink alcohol, or watch television, and are more likely to exercise. Other studies cited in the Jakobson et.al. article analyzed fiber intake, vitamins, or other factors. Another showed cardiovascular protective effects to religious orthodoxy. Any of these variables could be a confounding factor in the analysis, relating variables that shouldn’t be correlated.
In this study, as well as any observational study, there should be an understanding that a correlation of variables (such as lipid intake and CVD) do not necessarily prove a causative mechanism, especially considering the fact that there is no known mechanism as to why consumption of saturated fats could contribute to the development of CVD, except for the fact that they transiently raise blood cholesterol levels. On the other hand polyunsaturated fats, if consumed in excess, have potential toxicity and can certainly contribute to disease. When blood LDL levels are chronically elevated, lipoproteins are able to oxidize and contribute to an inflammatory condition that damages arteries. Based on this fact, it would be beneficial to consume fats that are less prone to damage. We must remember that any observational study can never be free from the bias of confounding factors, which can lead to erroneous conclusions. We don’t know if the source for saturated fat in the people chosen for these studies was coconut oil and spring butter (which is doubtful), or whether it came from trans-fats and fast-food hamburgers, which is more likely. The failure to make a distinction between a healthy saturated fats and unhealthy hydrogenated or trans-fats clouds the facts. Another wrench in the gears of this study is the fact that these “healthy” vegetable seed oils have actually been found to contain trans-fat! (O’Keefe, Gaskins-Wright, Wiley, & Chen, 1994) Extracting oil from vegetable seeds requires a tremendous amount of industrial ingenuity, which uses powerful chemicals and heat, which damages the delicate lipid structure, and leaves toxic residues behind. Another intellectual tar pit is the assumption that serum cholesterol levels are a proxy measurement for a person’s risk for heart disease; they are in some circumstances, but the relationship is not causal. I doubt it could be proven that consumption of coconut oil, butter, or grass-fed beef has any correlation to heart disease.
It should also be emphasized that Omega-3 and -6 oils are essential nutrients, but a protective effect of small amounts should not be extrapolated to suggest health benefits from mega-doses.
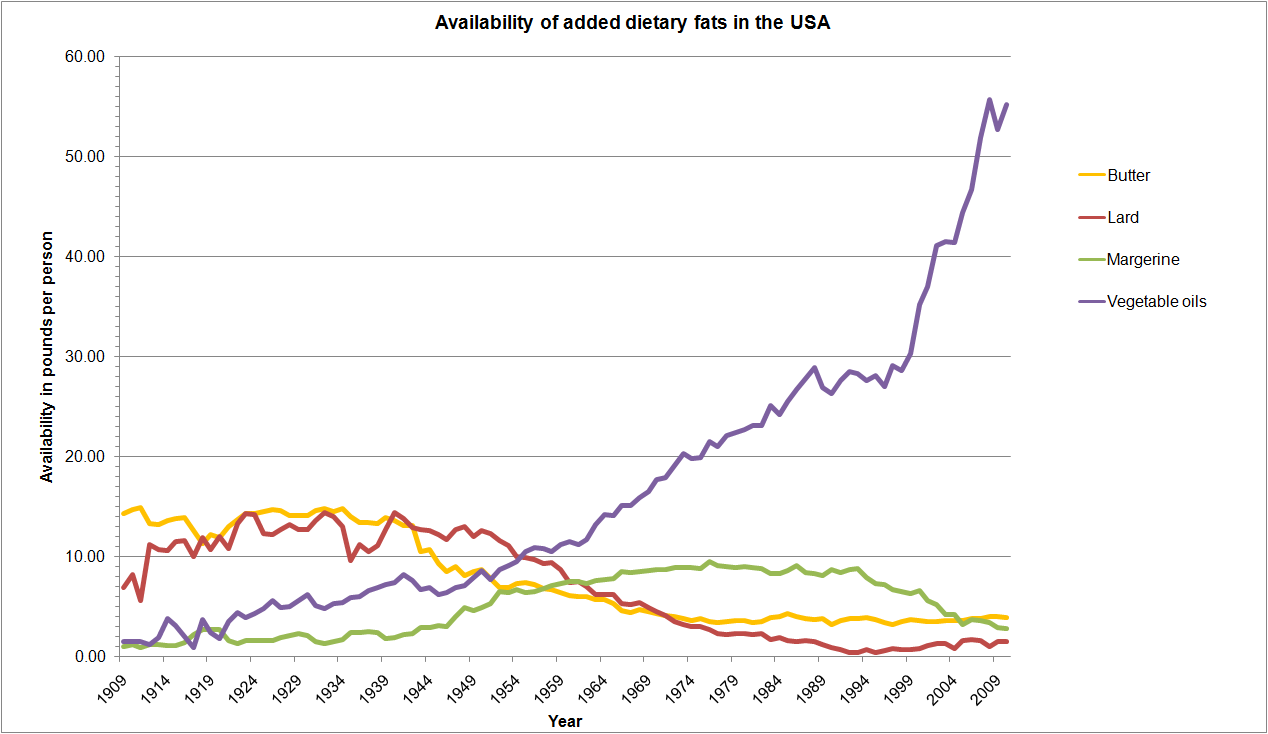
Yet the average American gets about 10% of calories from polyunsaturated fats, mostly in the form of refined vegetable oils. The increase in vegetable seed oil use is partly driven by the public policy of discouraging the consumption of animal fats. (Zegher, 2013)
Certain churches and religious traditions put emphasis on healthful diet, but the proponents of “Biblical” diets often have contradictory, and irrelevant conclusions, such as promoting veganism, or eating grains. Under the law of Moses, the consumption of animal fat and blood was prohibited [see Leviticus 7:23]. This has been used to support the anti-saturated fat campaign. The text actually prohibits the consumption of fat of cattle, sheep, and goats. The fat of these animals was reserved for the use in religious sacrifices. The text also prohibits consuming the blood of birds, but mention of fat is noticeably absent. No doubt there was good reason for these prohibitions, but it seems that people use the Bible to support a their ideas without ever having read the text. The Bible contains numerous casual mention of butter, cheese, and other traditional foods, many of which contain saturated fat.
In summary, saturated fats, even in significant quantities are healthful depending on their source, but perhaps not for everyone. Saturated fat increases the need for dietary choline, and in a choline and methionine deficient diet, the liver would have difficulty exporting fat (Masterjohn, 2010). Some people have a genetic defect that slows the processing of saturated fat, for example, people with the ApoE-4 gene. Less common mutations in the ApoB or ApoA gene may cause extreme elevations in blood cholesterol. Variations in the FTO gene affect risk for obesity or diabetes with high saturated, low polyunsaturated fat intake. Also, saturated fat is able to transport endotoxin across the gut barrier, which could cause serious complications for people with gut disbiosis (I’ll write more about this later). Animal fats could be correlated with disease risk because animal fat consumption is the primary source of certain toxins, particularly persistent organic pollutants. But for most people, reducing saturated fat intake to attempt to change cholesterol levels is treating a symptom of the problem, and ignoring the cause.
References:
Fraser, G., Sabate, J., Beeson, W., & Strahan, T. (1992). A Possible Protective Effect of Nut Consumption on Risk of Coronary Heart Disease. Retrieved from Jama Internal Medicine: http://archinte.jamanetwork.com/article.aspx?articleid=616417
Jakobsen et.al. (2009). Major types of dietary fat and risk of coronary heart disease: a pooled analysis of 11 cohort studies. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2676998/
Jaminet, P., & Jaminet, S.-C. (2012). Perfect Health Diet. Scribner.
Katan, M. B. (2009). Omega-6 polyunsaturated fatty acids and coronary heart disease. Retrieved from The American Journal of Clinical Nutrition: http://ajcn.nutrition.org/content/89/5/1283.long
Konstantinof, I., Mejivoi, N., & Anichkov, N. (2006). Nikolai N. Anichkov and His Theory of Atherosclerosis. Texas Heart Inst J.
Masterjohn, Chris. The Sweet Truth About Liver and Egg Yolks — Choline Matters More to Fatty Liver Than Sugar, Alcohol, or Fat https://chrismasterjohnphd.com/2010/11/23/sweet-truth-about-liver-and-egg-yolks/ 2010
O’Keefe, S., Gaskins-Wright, S., Wiley, V., & Chen, I.-C. (1994, September). LEVELS OF TRANS GEOMETRICAL ISOMERS OF ESSENTIAL FATTY ACIDS IN SOME UNHYDROGENATED U. S. VEGETABLE OILS. Retrieved from Wiley Online Library: http://onlinelibrary.wiley.com/doi/10.1111/j.1745-4522.1994.tb00244.x/abstract
Ornish, D. (2015, March 23). The Myth of High-Protein Diets. Retrieved from The New York Times: http://www.nytimes.com/2015/03/23/opinion/the-myth-of-high-protein-diets.html?_r=0
Ramsden, C., Zamora, D., Leelarthaepin, B., Majchrzak-Hong, S., Faurot, K., Suchindran, C., . . . Hibbeln, J. (2013). Use of dietary linoleic acid for secondary prevention of coronary heart disease and death: evaluation of recovered data from the Sydney Diet Heart Study and updated meta-analysis. Retrieved from BMJ: http://www.bmj.com/content/346/bmj.e8707
Rose, G., Thomson, W., & Williams, R. (1965, June 12). Corn Oil in Treatment of Ischaemic Heart Disease. Retrieved from British Medical Journal: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2166702/
Salatin, J. (1995). Salad Bar Beef. Swoope: Polyface, Inc.
Savory, A. (2013, February). Allan Savory How to fight desertification and reverse climate change. Retrieved from TED: http://www.ted.com/talks/allan_savory_how_to_green_the_world_s_deserts_and_reverse_climate_change?language=en
Tonstad, S., Stewart, K., Oda K., Batech, M., Herring, R.P., and Fraser, G.E. (2014 Apr 1) Vegetarian diets and incidence of diabetes in the Adventist Health Study-2 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3638849/
USDA, HHS. (2010). Dietary Guidelines for Americans 2010. Retrieved from Health.gov: http://www.health.gov/dietaryguidelines/dga2010/DietaryGuidelines2010.pd
Zegher, L. (2013, April 16). What happens when you take public health advice to heart? Retrieved from Supplement SOS: http://supplementsos.com/blog/taking-health-advice-to-heart/